Check out our entire series explaining the science involved in the coronavirus pandemic. Sign up to receive our coronavirus update each week.
How do scientists figure out how long the novel coronavirus remains infectious on surfaces?
Just when you thought you had enough to worry about, news comes out that the virus can remain infectious on surfaces for hours or days.
Okay, so how do scientists figure out how long coronavirus remains infectious on surfaces?
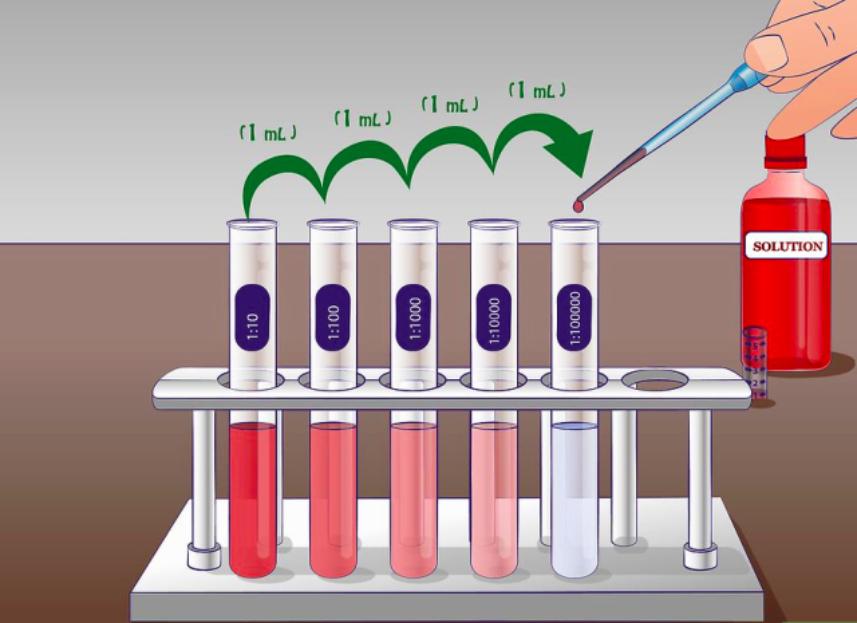
So glad you asked! Turns out, it’s all about serial dilution.
Ready?
Here’s the first part of the experimental procedure from the recent New England Journal of Medicine article that’s caused everyone to be anxious about touching anything outside their own homes:
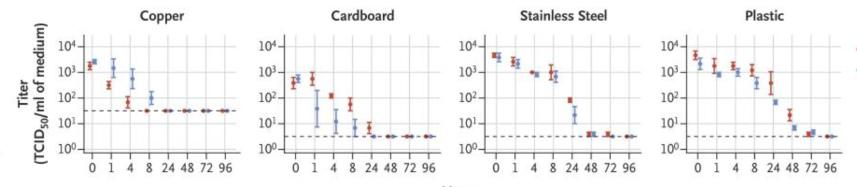
Aerosols (<5 μm) containing SARS-CoV-2 (105.25 50% tissue-culture infectious dose [TCID50] per milliliter) or SARS-CoV-1 (106.75-7.00 TCID50 per milliliter) were generated with the use of a three-jet Collison nebulizer and fed into a Goldberg drum to create an aerosolized environment.
Yikes. I’m not going to try to define all those terms. In plain language, the researchers took a whole lot of two different coronaviruses: SARS-CoV-1, which causes the disease SARS, and SARS-CoV-2, which causes the current pandemic of COVID-19. The researchers put a very specific amount of each coronavirus into a machine that mixed the virus with water and sprayed the resultant solution on various surfaces—copper, stainless steel, cardboard, and plastic. Then they took samples every hour and tested them on cultures of human cells. If cells died, the virus was still infectious.
That’s pretty simple, right? But you might wonder how they figure out how much of the virus is left at each time point.
To understand that, you have to dig into the term “TCID50,” which stands for Median Tissue Culture Infectious Dose. TCID50 is the amount of virus that kills 50% of the cells in a test tube or plated on petri dishes. When the description says the researchers started with 105.25 TCID50 per milliliter of SARS-CoV-2, that means they started with almost 200,000 times as much virus as they needed to kill 50% of your target cells.


 You will only get sick if you touch a contaminated surface and then touch your mouth or eyes. Wash your hands as soon as you arrive home!
You will only get sick if you touch a contaminated surface and then touch your mouth or eyes. Wash your hands as soon as you arrive home!